In Which of the Following Areas Can a Subcutaneous Injection Be Given?
Chapter 7. Parenteral Medication Administration
seven.3 Intradermal and Subcutaneous Injections
Intradermal injections (ID)are injections administered into the dermis, just beneath the epidermis. The ID injection route has the longest absorption time of all parenteral routes. These types of injections are used for sensitivity tests, such as TB (see Figure vii.13), allergy, and local anesthesia tests. The advantage of these tests is that the torso reaction is easy to visualize, and the degree of reaction can be assessed. The most mutual sites used are the inner surface of the forearm and the upper back, nether the scapula. Cull an injection site that is complimentary from lesions, rashes, moles, or scars, which may alter the visual inspection of the exam results (Lynn, 2011).
Equipment used for ID injections is a tuberculin syringe calibrated in tenths and hundredths of a millilitre, and a 1/4 to 1/two in., 26 or 27 gauge needle. The dosage of an ID injection is usually under 0.five ml. The angle of assistants for an ID injection is 5 to 15 degrees. One time the ID injection is completed, a bleb (small cicatrice) should announced under the skin. Checklist 56 outlines the steps to administer an intradermal injection.

Disclaimer: Always review and follow your hospital policy regarding this specific skill. | ||||
Condom Considerations:
| ||||
Steps | Additional Information | |||
| one. Fix medication or solution equally per agency policy. Ensure all medication is properly identified. Check physician orders, Parenteral Drug Therapy Manual (PDTM), and MAR to validate medication social club and guidelines for administration. | Properly identifying medication decreases adventure of inadvertently administering the wrong medication. Preparing medications ensures patient prophylactic with medication assistants.  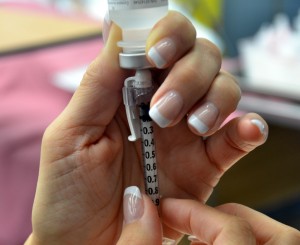 | |||
| ii. Perform mitt hygiene. | Assemble all supplies: medication syringe, non-sterile gloves, alcohol swab and sterile gauze, Band-aid (if required). 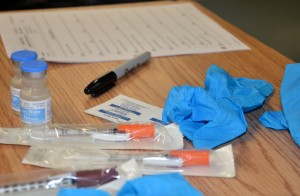 | |||
| three. Enter room and introduce yourself, explain procedure and the medication, and allow patient fourth dimension to inquire questions. | Explaining rationale increases the patient's knowledge and reduces their anxiety. | |||
| iv. Close the door or pull the bedside curtains. | This provides patient privacy. | |||
| five. Compare MAR to patient wristband and verify this is the correct patient using two identifiers. | This ensures accuracy of the medication or solution and prevents errors. Two patient identifiers are patient name and date of birth. 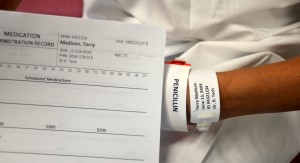 | |||
| 6. Assess patient for any contraindications to the medications. | Assessment is a prerequisite for every medication given. | |||
| 7. Select appropriate site for administration. Assist the patient to the appropriate position as required. | Site should be free from lesions, rashes, and moles. Selecting the correct site allows for accurate reading of the test site at the appropriate time. 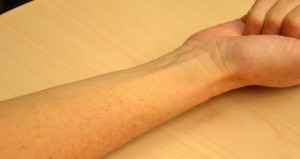 | |||
| viii. Perform hand hygiene and use non-sterile gloves. | Gloves assist prevent exposure to contaminants.  | |||
| 9. Clean the site with an booze swab or clarified swab. Use a house, circular move. Allow the site to dry out. | Pathogens from the skin can exist forced into the tissues by the needle. Allowing the peel to dry prevents introducing booze into the tissue, which can be irritating and uncomfortable. 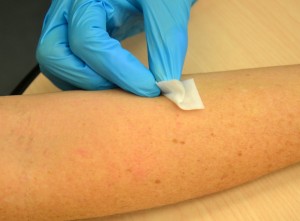 | |||
| 10. Remove needle from cap past pulling information technology off in a directly motion. | This decreases hazard of adventitious needle-stick injury.  | |||
| 11. Using non-dominant paw, spread the peel taut over the injection site. | Taut skin provides like shooting fish in a barrel entrance for the needle. 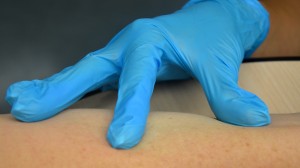 | |||
| 12. Agree the syringe in the dominant hand between the thumb and forefinger, with the bevel of the needle upward. | This allows for easy treatment of the syringe. 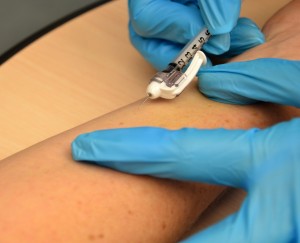 | |||
| 13. Hold syringe at a 5- to 15-degree angle from the site. Identify the needle virtually flat against the patient's peel, bevel side upwards, and insert needle into the skin. Insert the needle only nearly ane/iv in., with the entire bevel under the peel. | Keeping the bevel side up allows for smooth piercing of the pare and induction of the medication into the dermis. 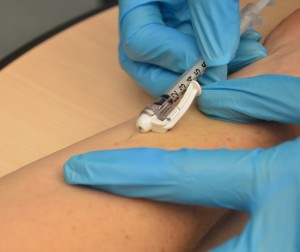 | |||
| fourteen. Once syringe is in identify, slowly inject the solution while watching for a small weal or bleb to appear. | The presence of the weal or bleb indicates that the medication is in the dermis. 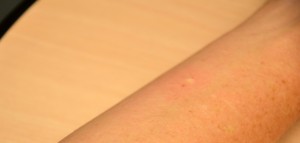 | |||
| 15. Withdraw the needle at the same angle as insertion, appoint safety shield or needle guard, and discard in a sharps container. Practise non massage expanse after injection. | Withdrawing at the same angle equally insertion minimizes discomfort to the patient and damage to the tissue. Proper needle disposal prevents needle-stick injuries.  Massaging the area may spread the solution to the underlying subcutaneous tissue. Gently pat with sterile gauze if blood is present. | |||
| xvi. If injection is a TB skin test, circle the area around the injection site to let for easy identification of site in three days. |  | |||
| 17. Discard remaining supplies, remove gloves, and perform hand hygiene | This prevents the spread of microorganisms.  | |||
| 18. Document the procedure and findings according to agency policy. | Proper documentation helps ensure patient safety. Document time, date, location, and type of medication injected. | |||
| xix. Evaluate the patient response to injection within advisable time frame. | The patient volition need to be evaluated for therapeutic and adverse effects of the medication or solution. | |||
| Data source: ATI, 2015a; Berman & Snyder, 2016; Brookside Associates, 2015a; Clayton, Stock, & Cooper, 2010; Perry et al., 2014 | ||||
Subcutaneous Injections
Subcutaneous (SC) injections are administered into the adipose tissue layer just below the epidermis and dermis. This tissue has few blood vessels, and so drugs administered by this road have a slow, sustained rate of absorption. Sites for SC injections include the outer attribute of the upper arm, the abdomen (from beneath the costal margin to the iliac crest) within ane inch of the umbilicus, inductive aspects of the thighs, upper back, and upper ventral gluteal surface area (Lynn, 2011) (run into Figure 7.fourteen).
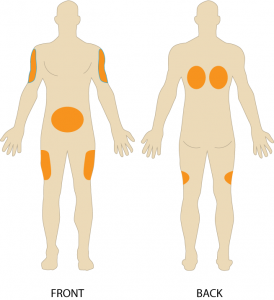
Choose a site that is free of skin lesions and bony prominences. Site rotation prevents the formation of lipohypertrophy or lipoatrophy in the pare. Physical exercise or application of hot or cold compresses influences the charge per unit of drug absorption by altering local blood menses to the tissues. Whatsoever condition that impairs that blood catamenia to the subcutaneous tissue contradicts the apply of subcutaneous injections. Examples of subcutaneous medications include insulin, opioids, heparin, epinephrine, and allergy medication (Perry et al., 2014).
To administrate an SC injection, a 25 to 30 gauge, iii/8 in. to 5/8 in. needle is used. Some subcutaneous injections come up prefilled with the syringe attached. E'er confirm that the right-size needle is advisable for the patient before utilize. Subcutaneous injections are usually given at a 45- to 90-degree bending. The angle is based on the amount of subcutaneous tissue present. Generally, give shorter needles at a ninety-degree angle and longer needles at a 45-caste angle (Lynn, 2011). SC injections do non demand to be aspirated every bit the likelihood of injecting into a claret vessel is minor. Usually, no more than i ml of medication is given subcutaneously, as larger amounts may crusade discomfort to the patient and may non be absorbed appropriately (Lynn, 2011).
There are varying opinions on whether to compression the skin during administration. Pinching is advised for thinner patients in order to lift the adipose tissue upwards and away from the underlying musculus and tissue. If pinching is used, release the pinch when the needle is inserted to avoid injecting into compressed tissue. Note, too, that elevating or pinching the pare has been institute to increase the risk of injury, as the needle may pierce the opposite side of the pare fold and enter the pare of the health care worker (Black, 2013). The abdomen is the best location for an SC injection if a patient has little peripheral SC tissue. If patient is obese, use a needle that is long plenty to insert through the tissue at the base of operations of the skin fold (Perry et al., 2014).
Insulin SC Injections
Insulin is considered a high-chance medication, and special intendance must be taken to ensure the correct amount of medication and type of insulin is administered at the correct time. Besides, prophylactic checks related to a patient receiving SC insulin should be carried out (Ellis & Parush, 2012). Table seven.five lists specific guidelines for administering insulin (and run across Figure 7.15).
| Insulin | Additional Data | ||
| Insulin is considered a high-risk medication. | Special care must be taken to ensure the correct amount of medication and type of insulin is administered, at the correct time. It is highly recommended to e'er get your insulin dosages double-checked by another wellness intendance provider. Always follow the standard for medication preparation at your agency. | ||
| Insulin is only administered using an insulin syringe. | Insulin is the merely drug with its ain type of syringe with a needle attached. Insulin is ever ordered and administered in units, based on a blood sugar reading and a diabetic insulin protocol (or sliding scale). Some hospitals have preprinted physician orders, and some hospitals accept handwritten orders. Insulin syringes can come up in 30-, 50-, or 100-unit of measurement measurements. E'er read the increments (calibration) advisedly. | ||
| There are dissimilar types of insulin. | In that location are rapid-, short-, intermediate-, and long-acting insulins. For each type of insulin, it is important to know how the insulin works and the onset, top, and duration of the insulin. | ||
| Administering two different types of Insulin. | If a patient is ordered 2 types of insulin, some insulins may be mixed together in one syringe. Many insulins MAY Non be mixed together. Do non mix Lantus (Glargine) or Levemir (Determir).If administering cloudy insulin preparations (Humulin – N), gently scroll the vial between the palms of your easily to re-suspend the medication. Ever depict up the short acting insulin first, to prevent it from existence contaminated with the long acting. If too much insulin is drawn up from the 2d vial, discard syringe and showtime over again. Always bank check with the PDTM for the well-nigh current guidelines regarding insulin administration.Insulin orders may change from day to day. Always ensure the most electric current physician orders are existence followed. | ||
| Know about rotating injection sites. | Injection site rotation is no longer necessary as newer insulins have a lower risk for hypertrophy of the skin. Typically, a patient will pick one anatomic area (e.thou., upper arm) and rotate the injection sites within that region to maintain consistent insulin absorption from day to 24-hour interval. Insulin absorption rates vary from site to site. The belly absorbs the fastest, followed by the arms, thighs, and buttocks. | ||
| Know when to administer insulin. | The timing of insulin injections is critical to right insulin administration based on blood saccharide levels and when the patient will eat. Knowing the elevation activeness and duration of insulin is critical to proper insulin medication management. If giving insulin, always ensure the patient is not nauseated, is able to consume, and that nutrient is arriving before the insulin starts working. Typically, short- or rapid-acting insulin is given xv minutes before meals. Intermediate- or long-interim insulin may be given twice daily, at breakfast and dinner. | ||
| Measure blood sugar levels and food intake. | Insulin injections are based on blood saccharide values and on when the patient will consume. The timing of an insulin injection is critical to ensure the patient receives insulin correctly. | ||
| Utilise insulin injection pens. | Injection pensare a new technology used past patients to self-inject insulin using a syringe, needle, and prefilled cartridge of insulin. It is essential that patients exist taught how to use injection pens and then they understand the technology. A mini-infusion pump is a bombardment-operated machine that delivers medications in very small amounts to patients with controlled infusion times. The most common types of mini-infusion sets are insulin pumps or subcutaneous infusion devices. For more information on mini-infusion sets and volume-controlled sets, see Suggested Online Resources in section vii.8. | ||
| Information source: Canadian Diabetes Association, 2013; Perry et al., 2014 | |||
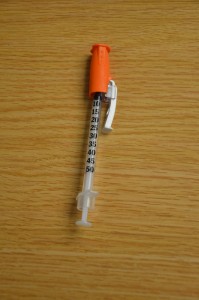
Special considerations:
- Insulin is stored in the fridge. When a vial is in utilize, it should be at room temperature. Do not administrate cold insulin. Cheque agency policy for how long a vial can exist used.
- Patients who accept insulin should monitor their blood carbohydrate (glucose) levels every bit prescribed by their health intendance provider.
- Vials of insulin should exist inspected prior to use. Any change in appearance may betoken a modify in potency.
- Use the type of insulin prescribed. Practise non modify the blazon unless ordered by a wellness intendance provider.
- Allow patient to choose site for injection. A patient may self-administer insulin if it's determined to be prophylactic and in the patient'due south best interest.
- All health care providers should exist enlightened of the signs and symptoms of hypoglycemia. Signs and symptoms include fruity breath, restlessness, agitation, confusion, slurring of words, damp peel, disability to concentrate or follow commands, hunger, and nausea. The patient may mutter of blurred or double vision. Late signs include unconsciousness. Hypoglycemia is a medical emergency. Always have an emergency diabetic kit available. If a conscious diabetic patient appears to exist hypoglycemic or has a claret sugar (glucose) reading of 4 mmol/Fifty or lower, requite glucose, such as sucrose tablets, solution, or juice. Follow agency policy regarding hypoglycemic reactions.
Heparin SC Injections
Heparin is an anticoagulant used to reduce the risk of thrombosis formation past suppressing jell germination (Perry et al., 2014). Heparin is likewise considered a high-alert medication (ISMP, 2014).
Table 7.vi provides specific guidelines to consider earlier and after administering heparin.
| Heparin | Boosted Data | ||
| Heparin is considered a loftier-run a risk medication. | Heparin is bachelor in vials and prefilled syringes in a multifariousness of concentrations. Because of the dangerous adverse furnishings of the medication, it is considered a high-run a risk medication. Always follow agency policy regarding the preparation and administration of heparin. | ||
| Rotate heparin injection sites. | Information technology is of import to rotate heparin sites to avert bruising in one location. To minimize bruising and pain associated with heparin injections, they tin be given in the intestinal area, at least 5 cm abroad from the navel. | ||
| Know the risks associated with heparin. | In that location are many risks associated with the administration of heparin, including bleeding, hematuria, hematemesis, bleeding gums, and melena. | ||
| Review lab values. | Review lab values (PTT and aPTT) before and afterward heparin assistants. | ||
| Use prepackaged heparin syringes. | Many agencies use prepackaged heparin syringes. Always follow the standards for safety medication administration when using prefilled syringes. Depression molecular weight heparin (LMWH) is more constructive in some patients. | ||
| Assess patient weather condition prior to administration. | Some conditions increment the risk for hemorrhage (bleeding), such as recent childbirth, severe diabetes, severe kidney and liver disease, severe traumas, cerebral or aortic aneurysm, cerebral vascular accidents (CVA), blood dyscrasias, and severe hypotension. | ||
| Assess medications prior to administration. | Over-the-counter (OTC) herbal medications, such as garlic, ginger, and horse chestnut, may interact with heparin. Additional medications that may collaborate include Aspirin, NSAIDS, cephalosporins, anti-thyroid agents, thrombolytics, and probenecids. | ||
| Data source: Clayton et al., 2010; Ogston-Constrict, 2014b; Perry et al., 2014 | |||
Checklist 57 provides the steps to complete a subcutaneous injection.
Disclaimer: Ever review and follow your hospital policy regarding this specific skill. | |||
Safety Considerations:
| |||
Steps | Boosted Data | ||
| 1. Set medication or solution equally per agency policy. Always compare the physician orders with the MAR. | Preparing medications ensures patient rubber with medication administration. 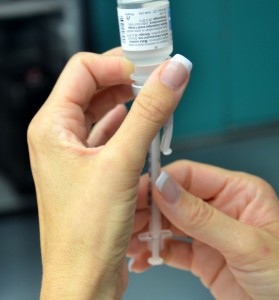 | ||
| 2. Perform manus hygiene; gather supplies. | You will need medication syringe, non-sterile gloves, alcohol swab and sterile gauze, Band-aid. | ||
| iii. Enter room and introduce yourself. Place patient using two acceptable identifiers, explain procedure and the medication, and let patient time to ask questions. | Explaining rationale increases the patient's knowledge and reduces their anxiety. | ||
| 4. Shut the door or pull the bedside defunction. | This provides patient privacy. | ||
| 5. Compare MAR to patient wristband and verify this is the correct patient using two identifiers. | This ensures accuracy of the medication or solution and prevents errors.  | ||
| vi. Assess patient for whatsoever contraindications for the medications. | Assessment is a prerequisite to the administration of medications. | ||
| 7. Put on non-sterile gloves. | Gloves help prevent exposure to contaminants.  | ||
| 8. Select appropriate site for administration. Assist the patient to the advisable position as required. | Site should be gratuitous from lesions, rashes, and moles. Choosing the correct site allows for accurate reading of the examination site at the appropriate time. 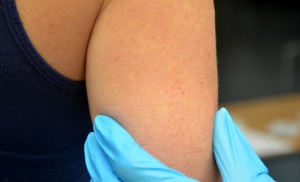 | ||
| 9. Clean the site with an booze swab or antiseptic swab. Use a firm, round motion. Allow the site to dry out. | Pathogens from the peel can be forced into the tissues past the needle. Allowing the skin to dry out prevents introducing alcohol into the tissue, which can be irritating and uncomfortable. 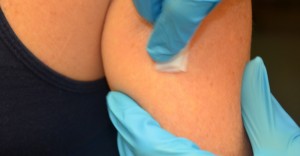 | ||
| ten. Remove the needle cap with the non-dominant hand, pulling information technology directly off. | This technique lessens the hazard of an adventitious needle-stick injury. | ||
| xi. Grasp or compression the area surrounding the injection site, or spread the peel taut at the site. | The decision to create a skin fold is based on the nurse's assessment of the patient and the needle length used. Pinching is brash for thinner patients. 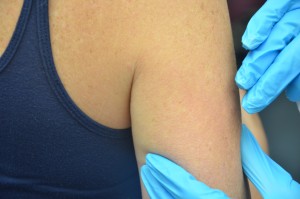 | ||
| 12. Hold the syringe in the dominant paw betwixt the thumb and forefinger. Insert the needle quickly at a 45- to 90-degree bending. | Inserting quickly causes less pain to the patient. Subcutaneous tissue is abundant in well-nourished, well-hydrated people. For patients with little subcutaneous tissue, it is best to insert the needle at a 45-caste bending. | ||
| 13. After the needle is in identify, release the tissue. Move your not-dominant hand to steady and lower the cease of the needle. With your dominant hand, inject the medication at a rate of 10 seconds per ml. Avert moving the syringe. | Keeping the needle steady helps keep the needle in place. 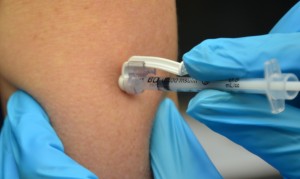 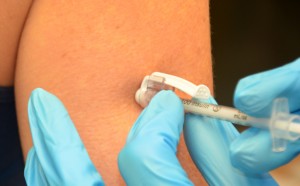 | ||
| fourteen. Withdraw the needle rapidly at the same bending at which it was inserted, while supporting the surrounding tissue with your non-ascendant hand. | Withdrawing at the same bending prevents tissue harm and increased pain at the injection site. | ||
| 15. Using a sterile gauze, apply gentle pressure at the site subsequently the needle is withdrawn. Practise not massage the site. | Massage is not necessary and can damage underlying tissue. Massaging subsequently a heparin injection can contribute to the formation of a hematoma. | ||
| xvi. Do not recap the needle. Apply the condom shield or needle guard on needle and dispose in a sharps container. | Safety shields and needle guards help prevent accidental needle-stick injuries. 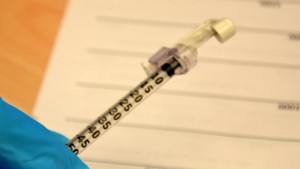  | ||
| 17. Dispose of supplies; remove gloves and perform mitt hygiene. | This reduces the risk of infection and the spread of microorganisms.  | ||
| 18. Certificate procedure and findings according to agency policy. | Timely documentation ensures patient safe. | ||
| 19. Evaluate patient response to medication. | It is important to evaluate the therapeutic outcome of the medication and assess for adverse effects. | ||
| Data source: ATI, 2015b; Berman & Snyder, 2016; Brookside Associates, 2015b; Clayton et al., 2010; National Institute of Health Clinical Heart, 2015; Ogston-Tuck, 2014b; Perry et al., 2014 | |||
Video seven.3
- Why should a wellness care provider rotate sites with a heparin SC injection, but only rotate within a site with insulin SC injections?
- What are 3 risks associated with administering insulin and heparin subcutaneously?
Additional Videos
Video 7.4
Source: https://opentextbc.ca/clinicalskills/chapter/6-7-intradermal-subcutaneous-and-intramuscular-injections/
0 Response to "In Which of the Following Areas Can a Subcutaneous Injection Be Given?"
Post a Comment